 
"I've done one patient and it worked," she explained. They discussed surgical options at length, then Skondra mentioned the drops. But in January 2017, now at UChicago Medicine, a new patient, a hospital administrator, came into her clinic with a small but full-thickness macular hole. She didn't try it again for almost a year since she did not have a patient that seemed to be a good candidate. 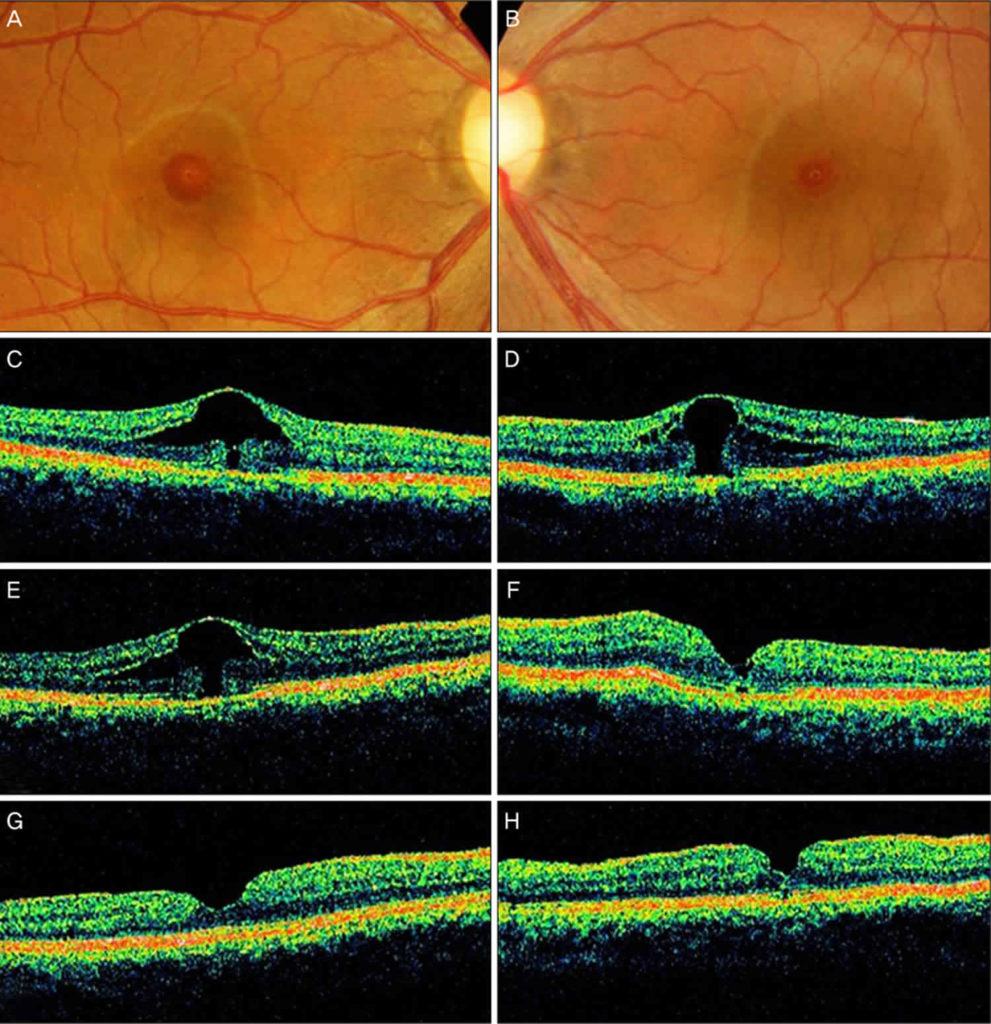
"If you Google this, you will not find it." The fact it got better with drops, worse after he stopped and then better after we restarted them is supporting the hypothesis that decreasing the swelling promotes hole closure as Dr Gentile's "hydration" theory suggested." "It worked, just as we hoped, and we avoided surgery. When he came back, Skondra put him back on the drops. Then, he went on vacation to Mexico and stopped using his eye drops. That drug, brinzolamide, helps pump fluid out of the eye to lower pressures for patients with glaucoma.Īll three were off-label uses, but they were unlikely to cause damage and "if the hole doesn't close," she reasoned, "we can still operate."Īfter two weeks, patient No. Then she added a third drug, an idea she got from a former mentor, Demetrios Vavvas, MD, PhD, an associate professor of ophthalmology at Harvard. She gave him two standard drugs: prednisolone, a steroid, and ketorolac, an anti-inflammatory. So, Skondra explained the eye-drop approach, and the patient was on board. He was afraid to have surgery since it was his only good eye. The patient in Chicago had only one good eye, and that eye had a small macular hole with swelling around it. "What an interesting idea," Skondra thought. He tried that on about ten patients and some of them recovered without needing surgery. As the fluid left and swelling decreased, the edges of the macular holes would sometimes creep back together, closing the hole. Instead of jumping straight to surgery, he sometimes gave patients two types of eye drops to dehydrate the retina and decrease the swelling around the hole. A speaker, Ron Gentile, MD, FACS, a professor of ophthalmology at the New York Eye and Ear Infirmary, mentioned that he was trying something new. She got the idea for the new approach at an ophthalmology conference. But if a surgeon does 100 procedures a year, Skondra points out, "that could mean some really unhappy and potentially visually disabled patients." This is uncommon, affecting only a small percentage of cases. There is also some risk that the surgery simply won't work, the hole will reopen or the retina will detach. It can take weeks to months for vision to improve depending on various factors like degree of cataract after a successful surgery. Patients with the bubble have to maintain a face-down position day and night for several days while the bubble - acting like an internal, temporary bandage - floats to the back of the eye, helping the edges of the hole approach each other leading to closure. There are always risks."Īt the end of the procedure, the surgeon inserts a gas bubble, designed to help close the hole. You operate on the retinal surface, a very delicate space. "Retinal surgery is always a serious surgery. This is a fairly straightforward operation when it comes to the vitreoretinal surgery spectrum "but it is retinal surgery," she said. Treatment has historically involved vitrectomy, a surgical process to remove the vitreous gel from the middle of the eye. Unfortunately, macular holes are common, especially for people over age 60. When someone with a macular hole looks directly at a face, they see a "big dark hole right in the middle," Skondra explained. Even a small gap in this delicate light-sensing tissue can cause blurred and distorted central vision. One of her clinical interests is the treatment of macular holes, a small unraveling of the macula, which is at the center of the retina.Ī functioning macula provides the sharp, clear, central vision people need to see fine details, to read or to drive. Terry Ernest Ocular Imaging Center at the University of Chicago, is a respected, board-certified retina specialist who focuses on the medical and surgical treatment of vitreoretinal diseases. Skondra, an assistant professor of ophthalmology and visual science and director of the J. 
"Not all retinal surgeons will like this because it decreases macular hole surgeries, one of the most commonly performed surgeries in a vitreoretinal practice." But we tried this on four patients and it worked for three of them. For the moment, this is just an idea, an off-label use of common drugs. "We haven't even designed, much less organized, a clinical trial - although we have an idea how we would like to set it up. "We haven't published anything yet," explained eye surgeon Dimitra Skondra, MD, PhD, about an experimental treatment. » View an updated story about eye drop treatment for macular holes 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
